Infliximab (Remicade) is a biologic medication licensed to be used in the treatment of Crohn’s disease and ulcerative colitis in adults and children. Find out more about it...
Remicade is the brand name for infliximab. It is a biologic medication made by the pharmaceutical company Janssen that is licensed to be used in the treatment of a variety of medical conditions including moderate to severely active Crohn’s disease and ulcerative colitis in both adults and children.
Crohn’s disease and ulcerative colitis have been linked to an increase in certain proteins - including one called tumor necrosis factor (TNF). Your body’s immune system naturally produces TNF.
An increase in TNF is linked to an increase in inflammation in the body’s digestive system - which can lead to a worsening of inflammatory bowel disease (IBD) symptoms.
Remicade is one of a group of medications which target TNF proteins, bind to them and block them. This helps to prevent inflammation in the body which is hoped will reduce IBD symptoms. The immune system is also suppressed. This can mean that people taking Remicade are more prone to picking up illnesses and infections.
Infliximab has been approved for use by:
Adults with Crohn’s disease
Children with Crohn’s disease
Adults with ulcerative colitis
Children with ulcerative colitis
You shouldn’t take infliximab if you have had heart failure, unless your doctor has examined you and decided you are able to receive it or if you have had an allergic reaction to infliximab or any of its ingredients.
Infliximab is an expensive medication and eligibility for it may vary depending on where you live. You may also find that during your treatment assessments need to be undertaken to see if you are still required to take it, due to its cost.
Before taking Remicade you should tell your doctor all of your symptoms and if you believe you may currently have any infections.
You should also tell your doctor if you are on any other medications, over-the-counter medicines, vitamins or supplements.
You should especially tell your doctor if you are taking:
If you are considered eligible to take infliximab your doctor will carry out some tests. This include tests for tuberculosis (TB) and hepatitis B. If these tests come back clear and your doctor has no other concerns then you may be eligible for infliximab.
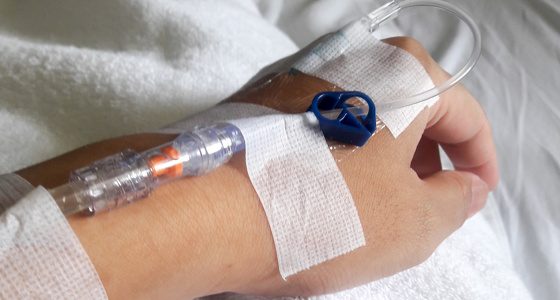
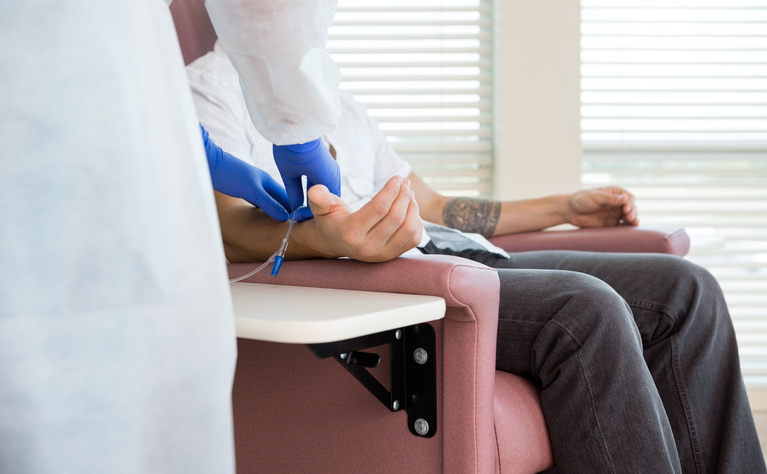
Infliximab is delivered via intravenous infusion (a needle placed in a vein in your arm). You will need to attend a hospital or a medical centre to receive this. The first three infusions are spaced close together (often referred to as loading doses) - usually at weeks 0, 2 and 6. After this you will receive an infusion approximately every 8 weeks.
Initially infusions will last around 2 hours, however this may be decreased if you have several successful infusions with no adverse reactions.
How long it takes to work, and whether or not it will work, varies from person-to-person. Some people report an improvement in symptoms after a few days, others up to 6 weeks after their first infusion.
Remicade affects your immune system and can lower its ability to fight infections.
The most common side effect of Remicade include:
More serious side effects can include:
People taking Simponi shouldn’t receive live vaccines or treatment with a weakened bacteria (such as BCG for bladder cancer).
Infliximab can interact with some other medications so it’s important that you tell your doctor about any medications you are taking before starting your infusions.
Biosimilars are biological medicines which are copies of the original licensed biologic medicine.
Biosimilars started being used in the UK after the patent for infliximab (Remicade) came to an end in February 2015, meaning any company is now allowed to copy the technology and research data used to make infliximab.
Inflectra and Remsima are both biosimilars of Remicade. They are both significantly cheaper than Remicade which means that some hospitals and medical centres are keen to switch patients to them. In some countries switching to a biosimilar drug can be done automatically without the patient’s knowledge. Current guidelines in the UK are that a patient’s consent must be gained. If you have any concerns, speak to your doctor.