Steph has been living with a stoma since May 2015. In this article she answers some common questions about what it's like to live with a stoma.
You can read Steph's full IBD story here.
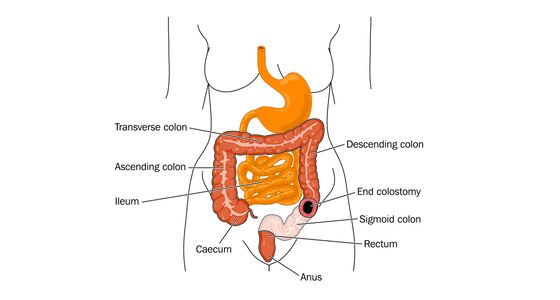
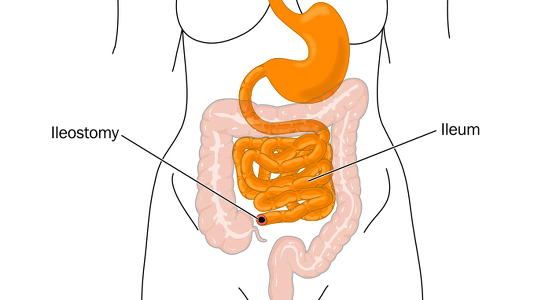
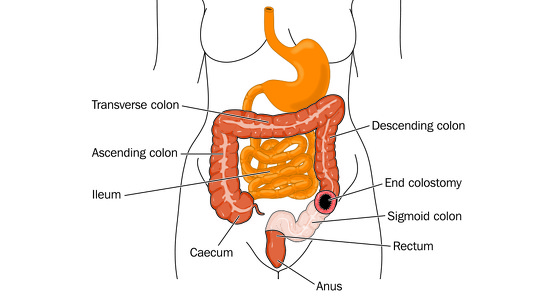
Q: What type of stoma do you have?
A: I have an ileostomy. 90% of my colon was removed during surgery and 10% was left incase I decided to go ahead with a reversal.
Q: When did you have it formed?
A: I've had my ileostomy since May 2015. I was 24 when my colon was removed.
Q: Why did you have it formed?
A: Mine was formed after a short battle with ulcerative colitis. I didn't have any previous symptoms, but two bouts of sepsis caused my UC to trigger. I only had four weeks of symptoms before my surgery.
Q: What was your initial reaction to your stoma?
A: I didn't look at my stoma for weeks. I was physically and mentally weak so I was fortunate to have the intensive care nurses help me change/empty it. I felt numb and didn't have many feelings towards it.
Q: How do you feel about your stoma now?
A: Me and Malcolm have a love-hate relationship. I love how he saved my life but sometimes I wish I could go back to before surgery. All the trauma of surgeries have taken their toll. Most days we are friends though.
Q: Have you named your stoma?
A: My stoma is called Malcolm, after the surgeon who formed him.
Q: How long did it take to recover from the surgery?
A: In total I spent 10 weeks in hospital. One week after my surgery I was rushed in for emergency surgery again. The stoma had been formed too tightly and nothing could pass through. Recovery in hospital seemed to be very slow, but as soon as I was home in my own bed and surroundings my recovery sped up. I slowly put some weight back on and adjusted to my new life.
Q: Did you have any complications?
A: Unfortunately I suffered from a lot of complications. I had a number of infections, mainly because I was so thin and had no immunity. I had a central line in my neck to feed me but this became infected so a new one was fitted. The next two central lines I had did the same and I spiked a temperature. The weeks after I left hospital I had two admissions with blockages. They both cleared by themselves with just some morphine to help me on the way. Two months after my original surgery I was admitted with "blockage" like symptoms. Unfortunately this one didn't unblock itself and adhesions from the surgeries were strangling my intestine, stopping anything from passing. I had to have surgery to removed the adhesions and within two weeks I able to go home again.
Q: What was it like to change your ostomy bag for the first time?
A: I was so excited to change my bag for the first time. I didn't do it until the day I was due to be discharged. I felt so proud once I'd done it and it came quite naturally.
Q: How long did it take to get used to caring for your stoma?
A: After my first bag change I felt really comfortable doing it and it just became part of my daily routine.
Q: What support from your hospital did you get in the early days?
A: Hospital support ended as soon as I left. My local stoma nurse took over straight away. I didn't see anyone from the hospital until my six week check up. I felt very alone. I went from 24-hour care to nothing and being at home and having to manage on my own.
Q: How often do you change your ostomy bag?
A: I change my bag every 3-4 days, even when I go swimming or shower/bath.
Q: Have you had any bag leaks? If so how did you deal with them?
A: I suffer with bag leaks quite a lot. Roughly 2/3 a month. It's part of having a stoma and for a few minutes I can feel cross and resentful towards my stoma but I quickly change it and get back to whatever I was doing.
Q: How do you deal with any noises from your stoma in public?
A: I always have a chuckle to myself when my stoma grumbles/pops. It doesn't bother me in the slightest. Sometimes I don't even realise it's doing it. I just slightly squeeze my bag and it stops.
Q: Do worry about smells from your bag? Do you do anything to try to control it?
A: I thought people who had ostomy bags of any kind smelt like faeces - until I had one myself! I don't get any smells from the bag until I empty it. I'm quite conscious of the smell even when i'm emptying it into my own toilet. I use a spray called Poo Pourri you spray it straight into the toilet bowl water and it's like magic! The smell disappears as soon as you flush. My one necessity.
Q: Are there any foods you have to avoid?
A: I eat most things, but like all ostomates there are certain foods that are a no-no for each individual. Mine are raisins/sultanas - they inflate to 10 times their size and then obviously struggle to pop out of the stoma. Sweet potato, popcorn and stodgy food tend to give me stomach pains so I avoid them.
Q: What has the reaction of your friends and family been like?
A: My family and friends have all been amazing. I've always had incredible support and most of them were just intrigued about how it worked and the cleverness of the bag. Without all these fabulous people I wouldn't have recovered as well as I have done.
Q: Do you tell new people about your stoma? How do you tell them?
A: I've always been a confident person and I've not really changed since my bag. I'm very open with people and always tell them about my stoma. I explain that I may look fine from the outside but hiding under my top is a bag that saved my life and just how proud I am of him and my scars.
Q: How has having a stoma affected your relationship with your boyfriend?
A: My relationship with my other half hasn't changed at all. If anything we are closer and happier than ever. We don't take each other for granted and any riffs are quickly resolved after realising how short life really is. Michael showed just how amazing he was through my hellish journey, he is one in a million and my rock.
Q: Is your son aware of your stoma and if so what questions does he ask and how do you answer them?
A: My little boy is 2 years 8 months and I had my stoma when he was 16 months. He is used to seeing my bag and calls its "mummy's poo poo". He knows what it's for but not quite why he hasn't got one too!
Q: What reaction do you get from people when they hear about your stoma for the first time?
A: I've always had positive comments towards my stoma. I'm not sure how I'd feel if I heard any nasty or rude things said about it, my confidence would be knocked a lot.
Q: Have you had to adapt the clothes you wear since have a stoma?
A: I've always loved fashion and clothes. I've continued to wear everything as I did before!
Q: Do you worry about your ostomy bag being visible under your clothing?
A: I make sure my bag is emptied fairly often to avoid it bulging out from the top of my jeans. I'm pretty sure no one would notice even if it was full up and sticking out though. More over I don't mind who sees it or what they say.
Q: What reaction have you got if you wear clothing which reveals your ostomy in public?
A: I always wear a bikini when I take my son swimming. Obviously people look, I think I would too. One person sniggered and whispered once. I didn't let it upset me and just carried on splashing around with my son.
Q: Can you still do they same physical activity that you did before?
A: I've never been one for exercise, even before the operation. Although, since my op I have climbed Mount Snowdon for charity and been to festival. I have a "go for it" attitude since my stoma. It hasn't and won't stop me doing anything. I'm fitter than I have ever been.
Q: How has having a stoma affected your life?
A: My life is the same as it was before. Physically I haven't changed. Mentally I think it will take me years and part of me thinks I will never get over what happened. The stoma doesn't upset or worry me. The surgeries, infections, time away from home etc still affect me now. Until a year ago I had nightmares but they slowly disappeared and I sleep much better now. 99% of the time I am absolutely fine and my life is normal. But there are days when I don't want to do this anymore, I don't want have a stoma anymore and the mental scarring gets the better of me. I feel like this is all a massive tragedy still. But it does pass and I'm Steph again.
Q: Do you currently take any IBD medication?
A: I take no medication at all and haven't since leaving hospital, apart from antibiotics on a few occasions.
Q: Do you still experience any IBD symptoms?
A: I suffer with bleeding and pain from my rectum still. I have ulcerative colitis in that part of my body still. I am due to have my rectal lining removed and my bag made permanent next year.
Q: What are your top tips for people who have recently had stoma surgery?
A: Be kind to yourself. Take thinks slowly and do one small thing you couldn't manage the day before e.g. making a sandwich, having a shower on your own etc to make your self confidence slowly return.
Don't be too adventurous with your diet in the first six weeks. You've been through a massive operation and trauma. Stick to soft, easily digestible food.
Don't be afraid to ask for help from family/friends or doctors if you're mentally struggling. Being teary and emotional is totally normally but you will adjust to your new addition. In weeks, months, years down the line you will realise just how amazing you are to get through what you did and be the person you are today.