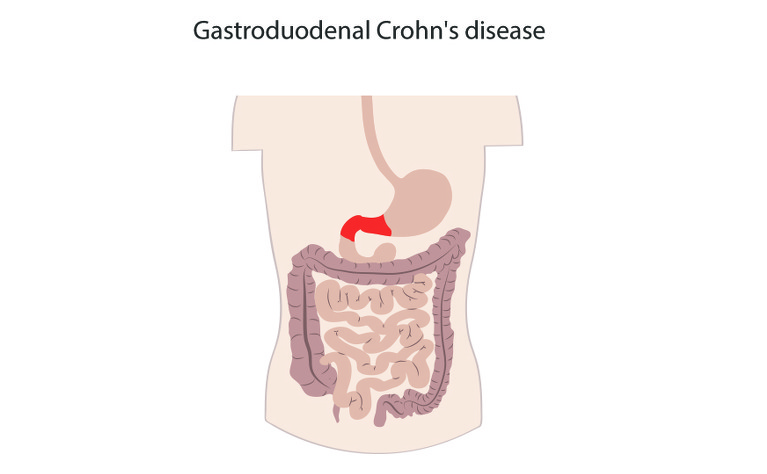
Gastroduodenal Crohn’s disease is a form of Crohn’s disease that causes inflammation to the oesophagus, stomach and/or duodenum (the first part of the small intestine).
Gastroduodenal Crohn's disease is not common - only up to around 5% of people with Crohn’s disease have gastroduodenal Crohn’s.
It is a lifelong chronic condition which cannot currently be cured and is part of a group of conditions known as inflammatory bowel disease (IBD).
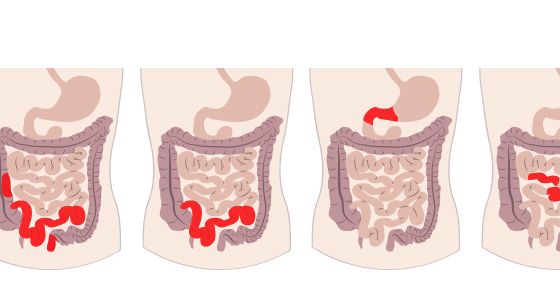
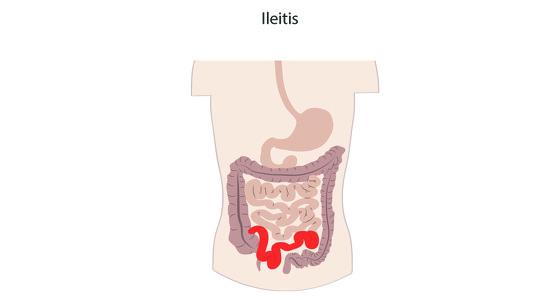
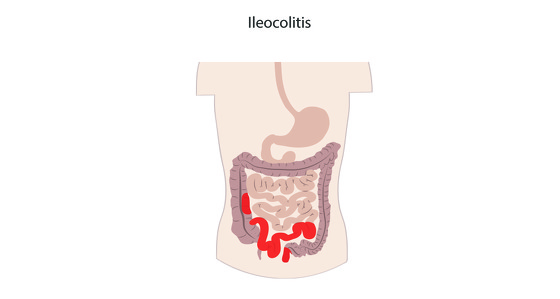
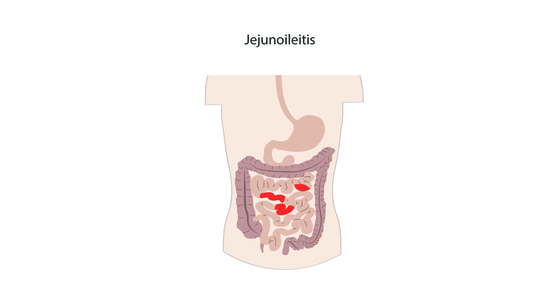
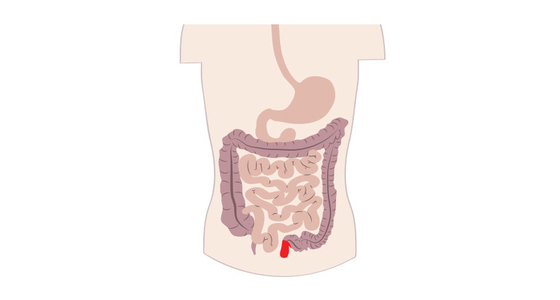
Crohn’s disease causes inflammation in the gastrointestinal (GI) tract. It most commonly affects the small intestine and the beginning of the large intestine, however it can affect any part of the GI tract from the mouth to the anus.
Crohn’s disease also affect the entire thickness of the digestive tract wall and may also skip areas - meaning you could have inflammation near you mouth and also in your small bowel but no where in between.
It is common for people with Crohn’s disease to be diagnosed with more than one type of the condition if inflammation is present in several places in the GI tract.
Typical symptoms include:
Treatments currently include medication and surgery. Some people have severely inflamed or damaged parts of their GI tract surgically removed. This can reduce or eliminate the symptoms, however it does not get rid of the disease and there is a risk that it will return to another area of the GI tract in the future.
Treatment may include acid suppression using a proton pump inhibitor as gastric acid can cause irritation in gastroduodenal Crohn’s.
Some people also make adjustments to their diet and lifestyle to support their medical treatment - such as exercise, improving quality of sleep, reducing stress.