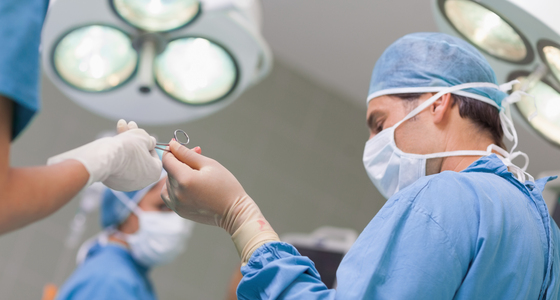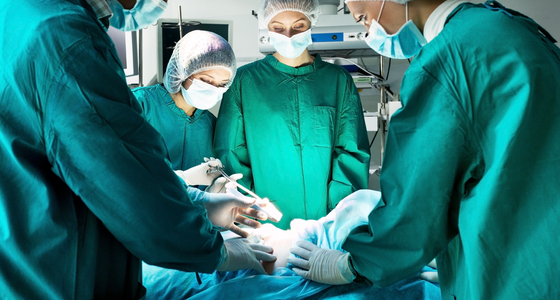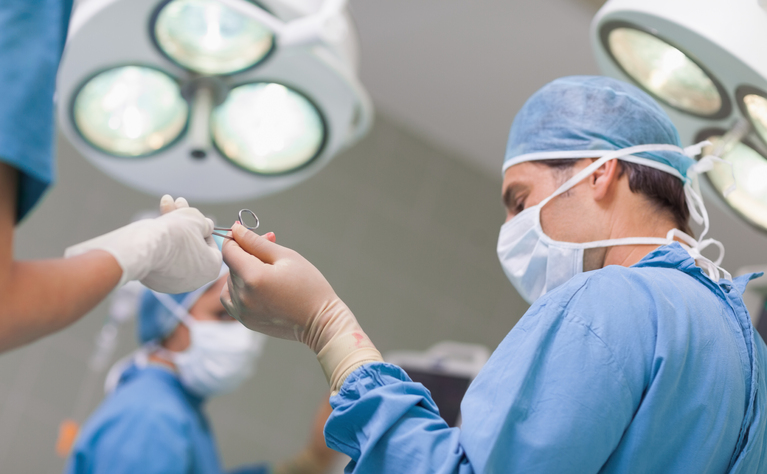
In percutaneous abscess drainage (PAD) surgery the abscess is drained using a catheter.
Abscesses are developed more commonly in Crohn’s disease but people with ulcerative colitis also develop them.
Abscesses are a common complication of Crohn’s disease and around 10-30% of people with the condition will spontaneously develop an abscess. They can also occur as a post-operative complication.
An abscess is an area that fills with pus and becomes red, swollen and painful. In people with Crohn’s disease they are most often found in the abdomen or the anal and rectal areas. In ulcerative colitis crypt abscesses can form in the colon.
Abscesses can often develop into fistula. This is more common in Crohn's disease.
As they can be painful surgery is used to get rid of an abscess.
Percutaneous abscess drainage (PAD) involves inserting a needle into the site of the abscess and then putting a catheter into it so that the fluid in the abscess can drain away.
The procedure will generally be done under local anaesthetic. Imaging technology is used to identify the position of the abscess. Once it has been found it takes between 20 minutes and an hour for the catheter to be put in place. The time it takes for the abscess to drain varies from person-to-person and can take several days. Once all the fluid has drained the catheter will be removed.
In general people receiving PAD stay in hospital for a few days, although everyone is different.